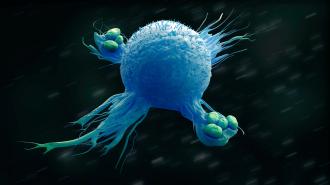
The human immune system is finely tuned to respond to a myriad of possible threats at a moment’s notice. Among the most important tools in its armoury are macrophages — white blood cells that engulf and destroy harmful microbes, cancer cells, and other invading objects which aren’t supposed to be there.
Unnecessary inflammation is known to be responsible for a wide array of chronic conditions.
This response is activated if macrophages detect pathogens nearby – but alternatively, if the danger is further away, they can trigger inflammation in the surrounding tissue. This can damage healthy cells, but also calls other macrophages closer to the threat into action, helping them to eliminate pathogens more quickly. Once the danger has passed, the cells will then send out molecular signals to switch off inflammation, allowing the tissue to heal.
Sometimes, unfortunately, the system goes haywire.
The challenge: Our immune system can’t always work perfectly. In some cases, it can even actively harm us, and attack healthy cells by mistake. In particular, unnecessary inflammation is known to be responsible for a wide array of chronic conditions: from arthritis and respiratory disease to diabetes and dementia.
Macrophages’ responses to nearby bacteria were strongly associated with a molecule named ribulose-5-phosphate.
Current treatments for these diseases tend to target proteins found on the outside of cells – but because the main molecular mechanisms employed by the immune system tend to take place inside cells, the success of these approaches has been limited so far.
Alternative treatments could be created by harnessing the mechanisms naturally used by macrophages to reduce inflammation when it is no longer needed. Until now, however, biologists haven’t identified the pathways followed by the cells as they discriminate between nearby and more distant threats, which can trigger inflammation.
Studying E. coli: A team of researchers in Australia may have just discovered the very molecule responsible for this crucial mechanism. In their study, biologists led by Kaustav Das Gupta at the University of Queensland, Brisbane, examined the responses of macrophages as they dealt with a particular strain of E. coli bacteria.
As they observed macrophages at varying distances from the pathogens, the team examined differences between the pathways followed by the cells as they discriminated between nearby and distant threats.
They discovered that their responses to nearby bacteria were strongly associated with a molecule named ribulose-5-phosphate – which instructed the cells to reduce their production of the molecular signals responsible for triggering inflammation.
New treatments could reduce unnecessary inflammation by kickstarting pathways that existed in our blood cells all along.
The healing pathway: Das Gupta and his colleagues propose that researchers could manipulate macrophages into producing higher quantities of ribulose-5-phosphate, creating an advanced new treatment for chronic inflammatory diseases.
The key to these treatments would lie with mRNA technology, which allows researchers to encode messages onto strands of RNA. Delivered into our cells, these mRNA messages would provide instructions for ribosomes (molecular machines inside our cells which assemble proteins). In this case, mRNA could instruct ribosomes to construct enzymes that catalyse the ribulose-5-phosphate reaction pathway.
By training immune cells in this way, Das Gupta’s team hope that new treatments could emerge that counteract its more harmful responses – reducing unnecessary inflammation by kickstarting pathways that existed in our blood cells all along.
As well as combating chronic inflammatory diseases, the researchers also hope their discoveries could lead to new breakthroughs in the ongoing fight against antimicrobial resistance. As harmful microbes become better at evading antibiotics, new techniques could train our immune systems to recognise and destroy them more easily.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].